SmartWound® PREDICT diagnostic dressing


Early, in-situ detection of wound infection
We are developing a prototype hydrogel wound dressing which respond to the cytotoxins secreted by bacteria in wounds as the wound becomes critically colonised with pathogenic bacteria.
The dressing (like the SmartWound-Resolve sensor) responds to the four primary wound microbes:
- Staphylococcus aureus
- Pseudomonas aeruginosa
- Candida species
- Enterococcus faecalis
Wound infection
Within seconds of injury, bacteria begin to colonise a wound. Most small wounds heal without infection, but some wounds become infected. The problem is there is no clinically accepted definition of wound infection.
The schematic (right), illustrates the change in a wound’s bacterial density when it is healing (blue line) or has developed an infection (red).
Note that the initial trajectory of infected and non-infected wounds are the same. The divergence point is the Critical Colonisation Threshold (CCT).


Detecting the CCT
The CCT is the earliest point in the wound healing / infection continuum at which wound infection can be detected. Our infection sensor contains phospholipid vesicles (left) dispersed in a gel matrix – these vesicles are lysed (broken open) by bacterial toxins secreted at the CCT. The vesicles contain a high concentration of a non-toxic dye, carboxyfluorescein, which becomes fluorescent when released from the vesicle.
The SmartWound® PREDICT dressing
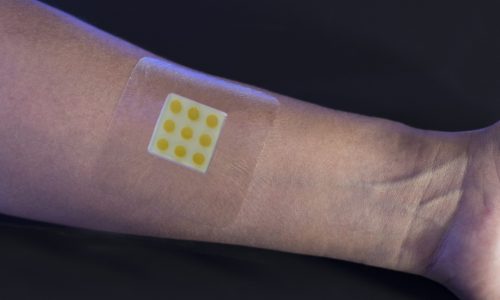
The dressing
An array of vesicle patches in a gel matrix. Comfortable to wear. Dressing and components are non-toxic and safe.

Initial research
The dressing research programme began in 2010 with funding from the European Commission, subsequently the EPSRC and Medical Research Council.

Development
The team consisting of scientists at the University of Bath and clinicians at Bristol Children’s Hospital and the QVH Hospital, East Grinstead has published over a dozen peer reviewed papers about the underpinning science.

Paediatric burns
The dressing should be effective for most acute and chronic wounds, but our initial patient focus is children with small scald burns. With 40,000 children in England & Wales annually suffering burns severe enough to need hospital attention each year.

South West Children's Burns Centre

Early warning prevents scarring, overuse of antibiotics and sepsis
We believe early warning of wound infection will lead to more effective, targeted treatment of patients with wounds and burns, resulting in less antibiotic prescription, reduced hospital stay and fewer complications such as sepsis.
References
[1] xxx

